More Children Were Covered by Medicaid and CHIP in 2021
The number of children under age 19 without health insurance fell to 3.9 million in 2021, according to the U.S. Census Bureau’s annual report on health insurance coverage released today.
That’s 475,000 fewer children without coverage than in 2020.
Health Insurance Coverage in the United States: 2021 shows that children received coverage from a variety of sources. Most children (61.9%) had private coverage primarily through their parents’ plan (Figure 1) but a growing share above the poverty level were covered by public programs.
Many lower-income children qualify for public health assistance programs, such as Medicaid and the Children’s Health Insurance Program (CHIP).
The uninsured rate among children decreased 0.6 percentage points to 5.0% between 2020 and 2021, driven by an increase in public coverage such as Medicaid and CHIP.
Medicaid provides health insurance coverage for children and adults with incomes below a certain income level. CHIP provides health insurance for children in families with income too high to qualify for Medicaid but likely can’t afford private health insurance.
In response to the COVID-19 pandemic, Congress increased funding for Medicaid and passed laws to keep individuals from losing Medicaid coverage during the national health emergency.
In 2021, Congress also introduced measures to increase access to care by reducing the cost of Health Insurance Marketplace coverage (created by the Patient Protection and Affordable Care Act or ACA). In addition, some states adopted measures to make it easier to apply for ACA coverage.
These changes may have contributed to the increase in health coverage of children — even those above the poverty level.
Medicaid and CHIP Drove Drop in Uninsured Rate 2020-2021
The uninsured rate among children decreased 0.6 percentage points to 5.0% between 2020 and 2021, driven by an increase in public coverage such as Medicaid and CHIP. Private coverage rates for children did not change between 2020 and 2021.
In 2021, 35.9% of children were covered by Medicaid or CHIP, up 1.2 percentage points from 2020. Between 2020 and 2021, the number of children covered by Medicaid or CHIP increased by an estimated 752,000.
Changes in the uninsured rate and in public coverage were not equally distributed across groups, however.
Medicaid and CHIP Coverage Increased for Children Above Poverty
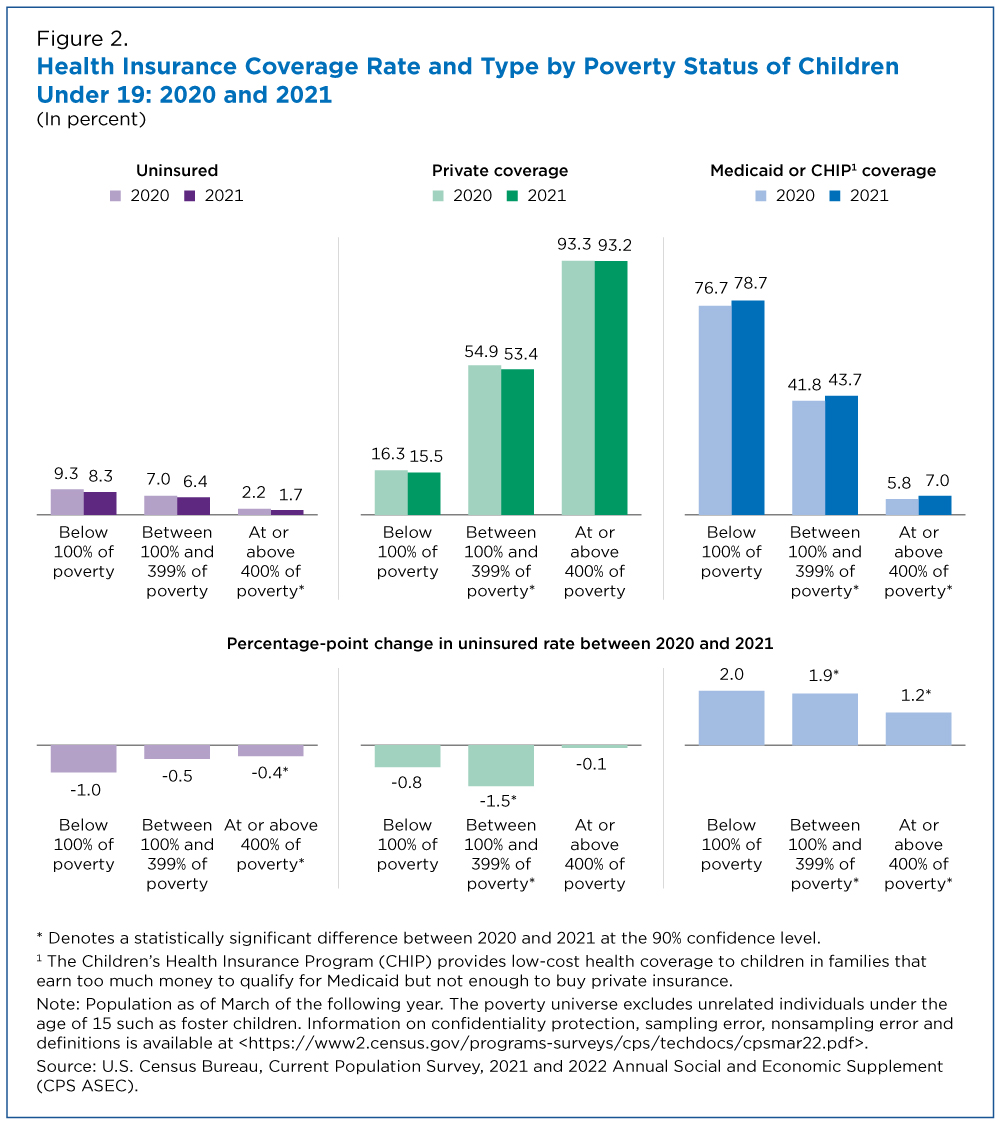
The income-to-poverty ratio provides a measure of family resources. Because Medicaid and CHIP programs are mostly available to families with fewer resources, Medicaid and CHIP coverage rates decline as the income-to-poverty ratio increases. On the other hand, private coverage rates increase as income-to-poverty ratio increases (Figure 2).
But expanded public programs during the pandemic may have contributed to a 0.4 percentage-point drop in the uninsured rate for children in families with incomes at or above 400% of poverty (the poverty threshold in 2021 was about $27,479 for a family with two parents and two kids).
There was no change in private coverage, but coverage through Medicaid and CHIP for this group increased by 1.2 percentage points, and 7.0% of children in this group were covered by Medicaid or CHIP in 2021.
Although the uninsured rate for children fell overall between 2020 and 2021, there was no change in the uninsured rate for children in families most likely to be eligible for coverage through public programs: those with incomes below poverty or in the middle income-to-poverty category (family income between 100% to 399% of their poverty threshold).
For children in poverty, there was no change in either private coverage or Medicaid and CHIP coverage rates between 2020 and 2021. A 1.9 percentage point increase in Medicaid and CHIP coverage rates offset the 1.5 percentage point drop in private coverage of children in the middle-income category during this period.
Medicaid Expansion and Children’s Health Insurance
Where a child lives may also affect their health insurance coverage.
In 2021, 36 states and the District of Columbia expanded Medicaid eligibility (“expansion states”) under the ACA to extend health coverage to low-income families. The remaining 14 states had not expanded eligibility (“nonexpansion states”) on or before 2021.
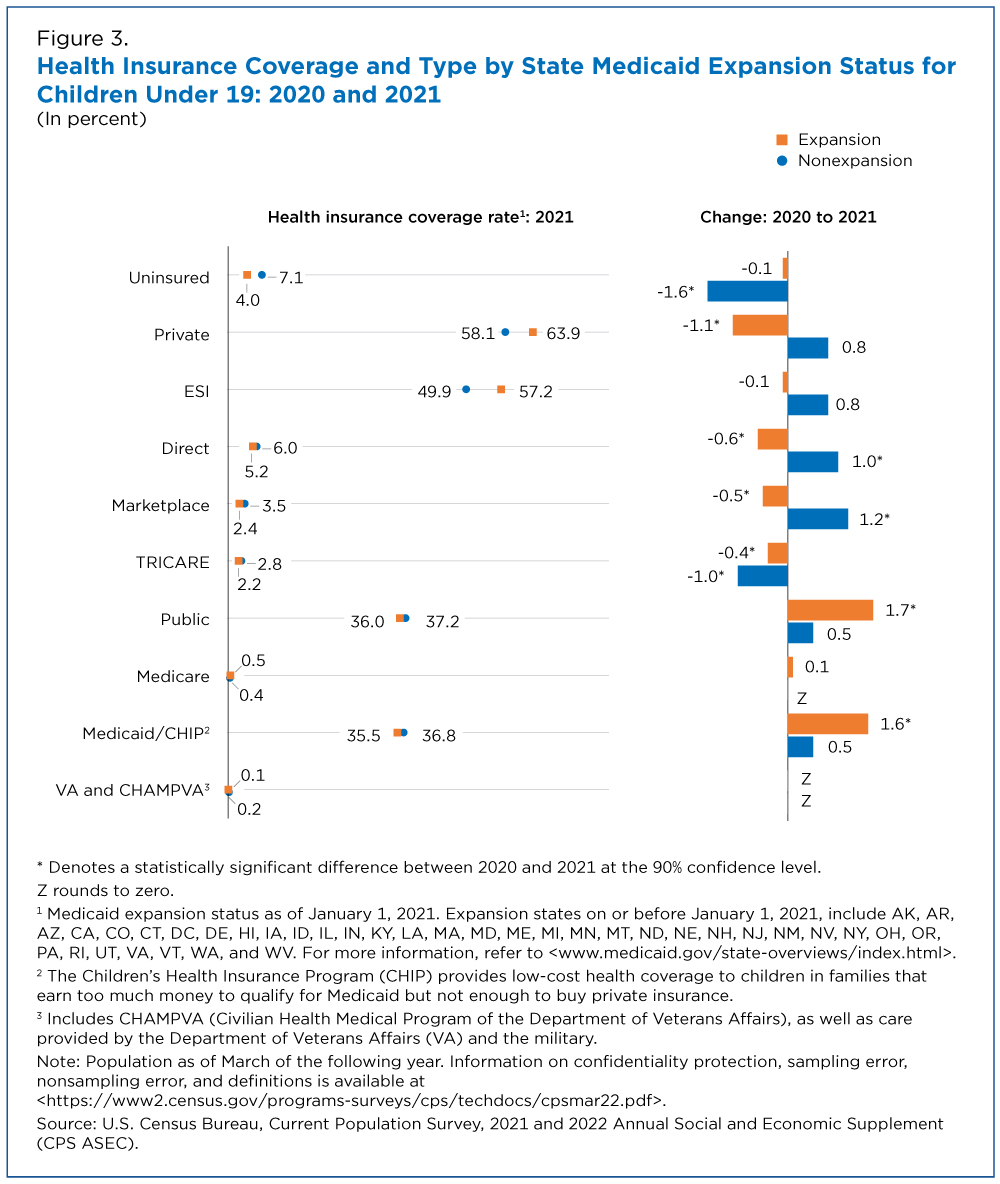
In 2021, about 50 million children lived in expansion states, and 27 million in nonexpansion states. About two million (4.0%) children in expansion states and 1.9 million (7.1%) in nonexpansion states did not have health coverage (Figure 3).
The uninsured rate for children living in nonexpansion states decreased by 1.6 percentage points from 2020 to 2021, driven in part by changes in children’s direct purchase coverage in these states.
Direct purchase coverage rates for children in nonexpansion states increased by 1.0 percentage points to 6.0% during this period, including coverage purchased through the Marketplace which increased by 1.2 percentage points to 3.5%.
There was no change in the number or percentage of children covered by Medicaid or CHIP in nonexpansion states.
The uninsured rate of children living in expansion states did not change between 2020 and 2021.
Although Marketplace coverage fell by 0.5 percentage points, Medicaid and CHIP rates rose 1.6 percentage points to 35.5% in expansion states. In 2021, about 691,000 more children in expansion states were covered by Medicaid or CHIP than in 2020.
Changes in health insurance coverage may result from several factors, including demographic changes in the population, changes in economic conditions, and changes in federal and state policy which impact access to care.
Policies to improve access to care during the COVID-19 pandemic may also have contributed to lower uninsured rates for children, as more children in expansion states received coverage through Medicaid and CHIP, and those in nonexpansion states through the Marketplace during the national emergency.
Related Statistics
-
Stats for StoriesNational Health Center Week: August 6-12, 2023The 2021 County Business Patterns program counted 54,642 outpatient care centers in the U.S. with 1,225,333 paid employees and an $84.1 billion annual payroll.
-
Current Population Survey (CPS)The CPS is a monthly survey sponsored by the Bureau of Labor Statistics and conducted by the U.S. Census Bureau.
Subscribe
Our email newsletter is sent out on the day we publish a story. Get an alert directly in your inbox to read, share and blog about our newest stories.
Contact our Public Information Office for media inquiries or interviews.
-
America Counts StoryFull-Time, Year-Round Workers More Likely to be Uninsured in 2021September 13, 2022The uninsured rate of those who worked less than full time, year-round dropped 1.2 percentage points from 2020 to 2021 as public coverage increased.
-
America Counts StoryGovernment Assistance Lifts 45.4 Million Out of Poverty in 2021September 13, 2022The 2021 U.S. official poverty rate of 11.6% was not statistically different from 2020 but the Supplemental Poverty Measure at 7.8% was lowest on record.
-
America Counts Story2021 Income Inequality Increased for First Time Since 2011September 13, 2022U.S. Census Bureau’s income data released today show widening income inequality from 2020 to 2021.
-
America Counts StoryChild Poverty Fell to Record Low 5.2% in 2021September 13, 2022In 2021, child poverty rates measured by Supplemental Poverty Measure were the lowest since 2009 for all race and Hispanic origin categories examined.
-
PopulationEight of the Nation’s Top 15 Last Names Stayed the Same Since 1790April 14, 2026Newly released names data from the 2020 Census show which first and last names are the most popular across the nation.
-
AgeU.S. Population Aging as Nation Turns 250April 09, 2026New population estimates show women still outnumbered men at older ages, but the gap is narrowing due to lower mortality rates and historical factors.
-
Business and EconomyState Lottery Ticket Sales Soar as Prizes Get LargerApril 08, 2026While sales nearly doubled to $104.7 billion from 2008 to 2024, state lottery prizes more than doubled to $34.5 billion in FY 2024.
-
Families and Living ArrangementsNumber of Same-Sex Couple Households Nearly Doubled From 2005 to 2024April 01, 2026Census Bureau data show demographic and economic characteristics of same- and opposite-sex couple U.S. households.